
How St. Luke’s Turned Medication Access Into a Strategic Advantage
.jpg)



At most health systems, medication access work sits quietly in the background often taking the form of growing backlogs, delays in care and missed opportunities. In practice, it shapes how quickly patients start therapy, how consistently teams execute, and whether the health system captures the value of the care it delivers. The medication access team and their clinical knowledge directly impact the patient experience. St. Luke’s Health System recognized that this work was an untapped strategic opportunity and approached it differently.
Rather than simply asking how to accelerate prior authorizations, St. Luke’s asked a more fundamental question: how should medication access be designed so it improves patient access, adherence, and enterprise growth?
To answer that question, St. Luke’s partnered with Latent Health to deploy AI-enabled prior authorization and appeals automation across both pharmacy and medical benefits. But the real transformation came from redesigning the work, centralizing the execution and giving teams better visibility into the medication access work.
The result was a stronger operating system. This shift transformed medication access from a reactive, backlog-driven function into a proactive, capacity-driven model aligned to patient outcomes and enterprise growth.

Redesigning the Work Before Automating It
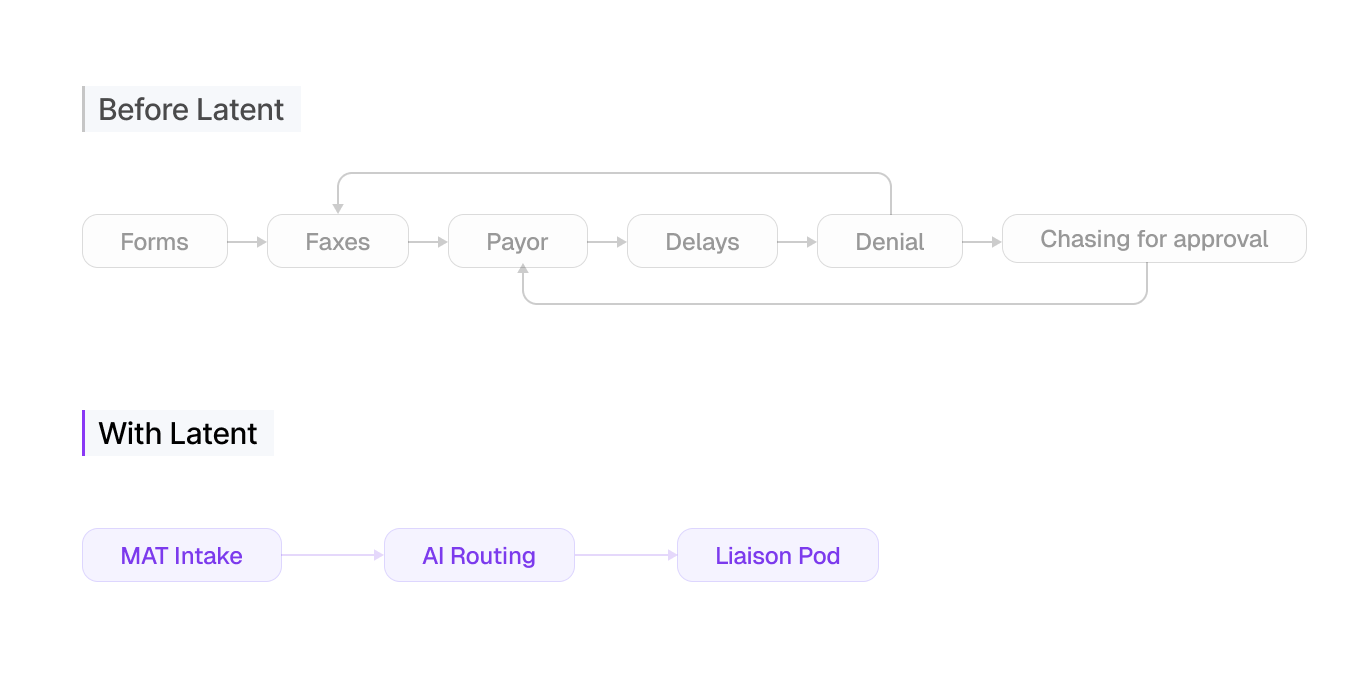
A critical insight that guided the partnership early was: AI amplifies the system it is placed into. If workflows are fragmented, AI accelerates fragmentation. If workflows are optimized, AI accelerates growth.
Before implementation, St. Luke’s had already aligned around a centralized Medication Access Team (MAT), reshaping intake and triage around a more structured, proactive system. The team moved into pod-based execution, with each pod made up of 3 to 5 FTEs focused on 1 to 2 disease states and the clinics and medications associated with them.
Leadership also made a deliberate decision to not reduce staffing, so the same team could be redeployed as patient advocates and centralized pharmacy liaisons to drive care coordination & internal script capture.
Speed as a Clinical and Financial Lever
Implementation was rapid. The Latent platform was live within five days of IHT build time, integrating directly into existing workflows without disrupting clinical operations. Almost immediately, the impact signals became visible.
What had historically taken over 7 days, began trending toward a 3-day PA Turnaround Time (TAT). Clinical review times dropped >72% from 18 minutes to 5 minutes per PA. With the same MAT FTE base, the team began processing over 1,200 additional PAs per month.
Those efficiencies meant fewer abandoned prescriptions, less delays, and faster starts to therapy minimizing how many patients were lost during critical access moments. Critically, it also created the capacity to intervene earlier in the patient journey when decisions about where prescriptions are filled are still being made & link patients to internal pharmacies.

From Transactions to Patient Advocacy
As repetitive work moved out of the way, the role of the Medication Access Team began to evolve. Instead of functioning as processors of administrative tasks, team members shifted to centralized liaisons engaging patients, coordinating care, and guiding prescriptions into St. Luke’s specialty and retail pharmacy network.
The operational impact was visible in backlog performance as well: during the January to March 2026 period, average backlog was 33% lower than the year before, giving the team more room to stay ahead of work and spend more time on patient-facing coordination.
This shift is critical, because health systems consistently see higher adherence rates, better outcomes, and stronger financial performance when prescriptions are retained within their integrated pharmacy ecosystem & larger integrated delivery network.
This transformation matters because it changed how value was created and reframed the MAT from a cost center into a growth engine while directly influencing capture rate, adherence, and patient experience (NPS scores).
Visibility Changed the Improvement Cycle
Latent’s reporting layer changed how St. Luke’s could manage the work. Structured, real-time reporting provides access to provider-level approval rates, review times, and payer-specific trends. These insights reveal patterns that were previously hard to quantify: variability in documentation practices, inconsistent ICD-10 coding, and prescribing behaviors that inadvertently trigger unnecessary prior authorizations.
This level of transparency enables targeted interventions such as refining documentation templates and smart phrases, educating providers, and aligning medication selection with payer requirements such as preferred agents, step therapy protocols, and appropriate days’ supply.
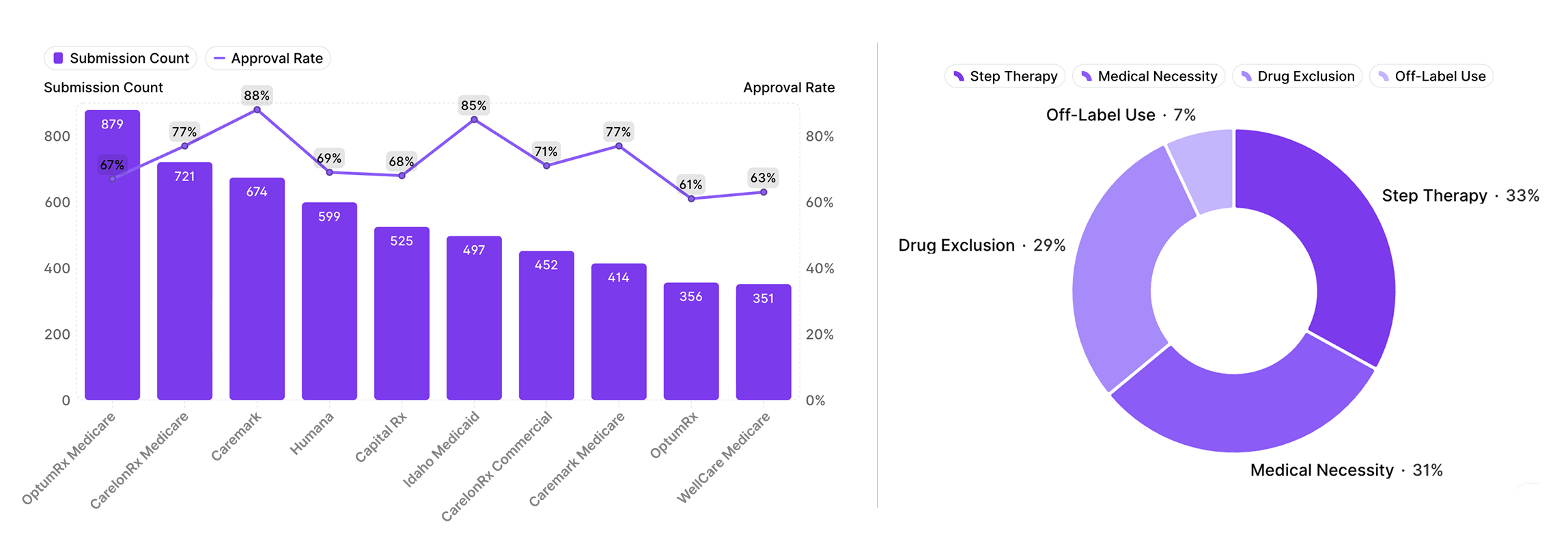
AI did more than reduce manual work. It made continuous improvement more specific and more operational by diagnosing systemic inefficiencies.
ROI Was Broader Than Labor Savings
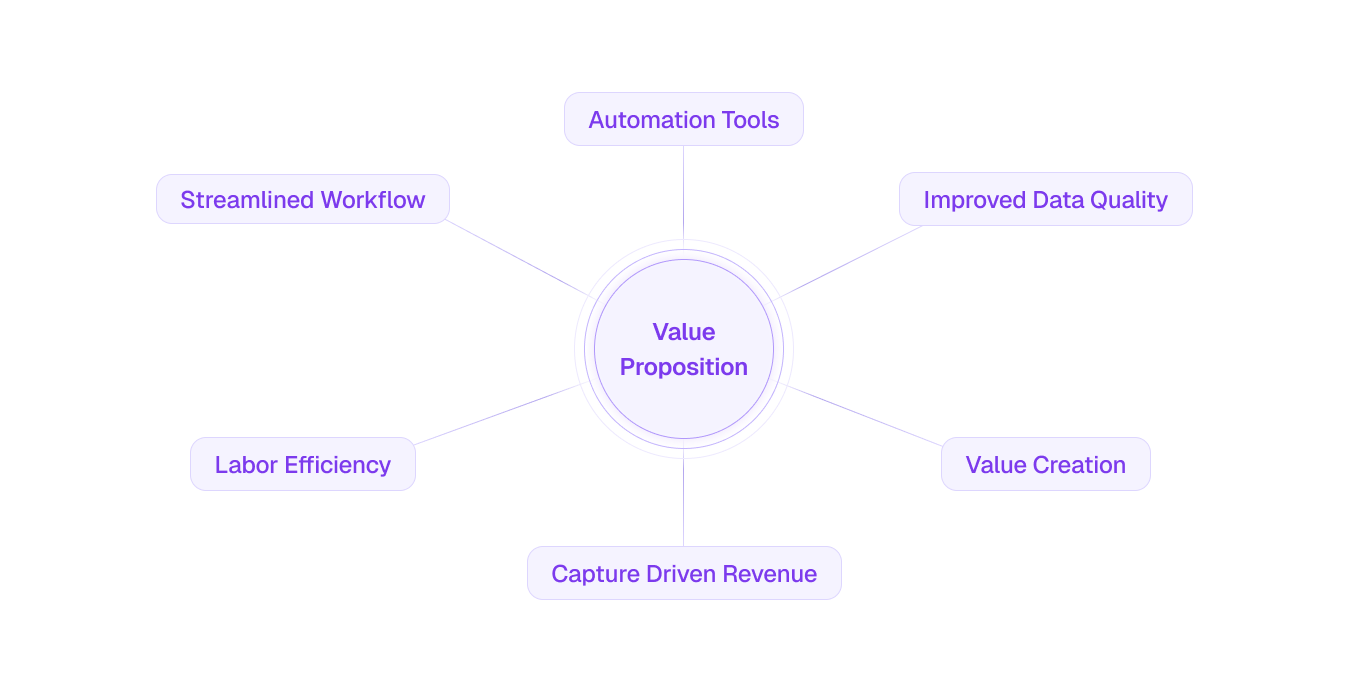
The financial impact of this transformation was both immediate and compounding. The increased capacity, and accelerated turnaround times enabled earlier patient engagement, which unlocked downstream value through improved prescription capture, refill retention rates, and patient adherence.
Organizations like St. Luke’s can expect multi-million dollar annual value creation, driven primarily by revenue capture acceleration rather than labor reduction alone. This type of transformation typically delivers:
- Strong multi-fold return on investment (ROI) within the first year
- Rapid payback period measured in months, often within the first quarter post-implementation
- Ongoing, compounding returns driven by refill retention and longitudinal patient engagement
Defining a True Partnership
What distinguishes these results is the shared understanding of the work itself: medication access is not simply administrative throughput. It is clinical execution that depends on surfacing the right patient-specific evidence, aligning it to payer requirements, and moving cases forward with consistency.
Latent and St. Luke’s operated with shared accountability, aligning on outcomes rather than outputs. Workflow redesign preceded automation, so the technology was applied to a stronger operating model rather than layered onto fragmentation. Feedback loops were rapid and continuous. Success was measured by patient access, financial performance, and staff experience.
A Blueprint for the Future
The experience at St. Luke’s offers a clear lesson for health systems navigating similar challenges. Benefits investigation, prior authorization, and appeals do not have to remain isolated administrative burdens. When health systems redesign the work, centralize ownership, and pair operational discipline with AI, medication access can become faster, more consistent, and more valuable to the organization.
For leaders thinking about the future of pharmacy operations, the question is no longer whether these workflows should be modernized. It is how quickly they can be redesigned to support better access, better execution, and stronger long-term performance.
Their model is now positioned to scale across additional service lines and disease sates, establishing a repeatable workflow on a platform built for enterprise-wide scalability. This is a blueprint for the future of health system medication access, not just an AI investment story.






